Why Do I Feel Dizzy When I Stand Up? Common Causes, What to Do, and When to Get Help
If you've ever stood up from bed, the couch, or a chair and suddenly felt woozy, faint, or unsteady, you're not imagining it. A brief drop in blood pressure is a common reason, especially in older adults and in people who take blood pressure medication. Here's what may be happening, what to do in the moment, and the signs it's time to get medical help.
Quick Takeaways
- A common cause of dizziness after standing is a brief drop in blood pressure called orthostatic hypotension. [1][2]
- Dehydration, blood pressure medication, illness, long periods of sitting or lying down, and anemia can all contribute. [1][3]
- Sit or lie down right away if you feel faint.
- If it happens often, causes falls, or comes with red-flag symptoms, get medical care.
If you stand up and feel lightheaded for a few seconds, you're not alone. It can be unsettling, especially if you have to grab a wall, sit back down, or wait for the feeling to pass.
In many cases, this happens because your blood pressure drops briefly when you change position. Your body usually corrects it quickly. But if it keeps happening, causes falls, or comes with symptoms like chest pain, fainting, or shortness of breath, it should not be brushed off. This article is for education, not a diagnosis, but it can help you understand what may be going on and what to do next.
What's happening in your body
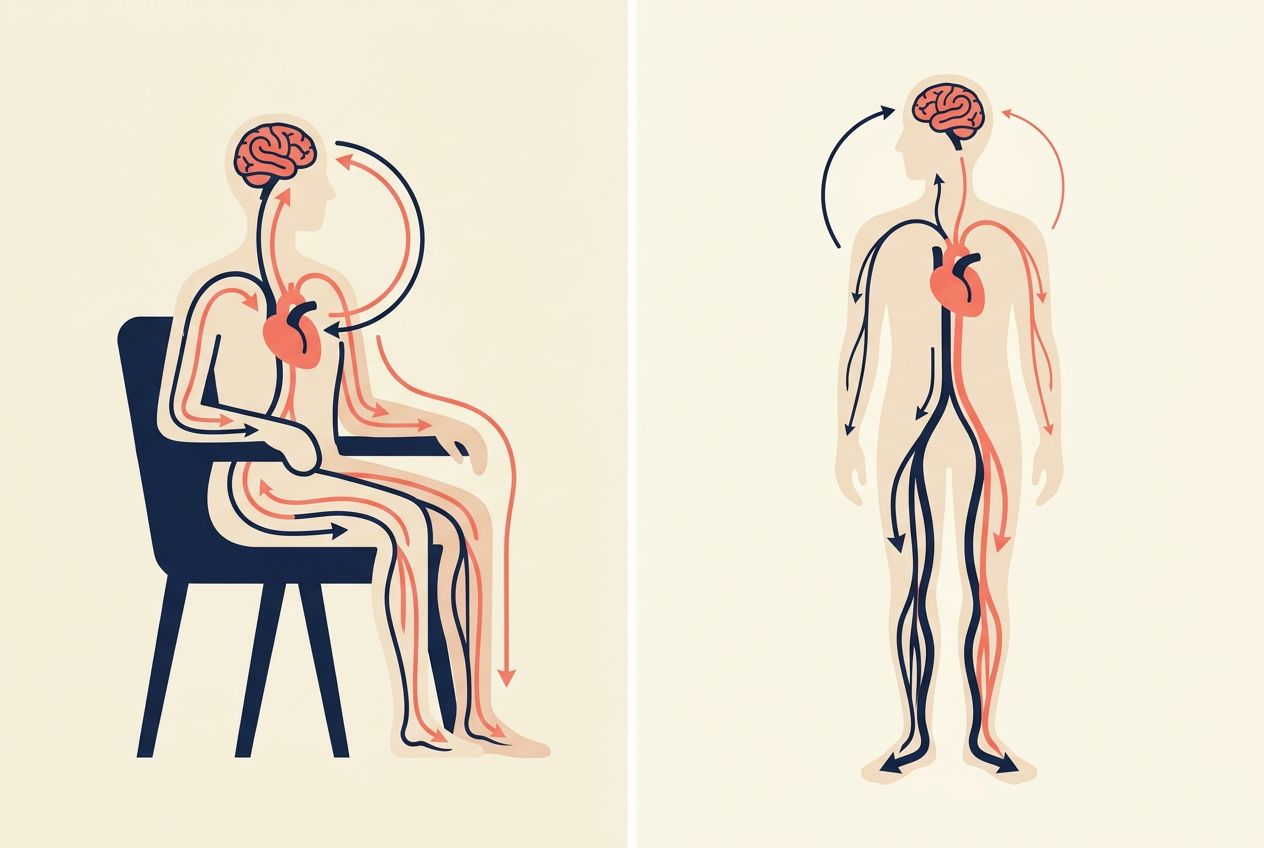
When you stand up, gravity pulls blood toward your legs and lower body. Normally, your blood vessels tighten and your heart rate adjusts fast enough to keep blood moving to your brain. [3]
When that adjustment is too slow or not strong enough, blood pressure drops for a moment. Less blood reaches your brain, and you may feel lightheaded, weak, dimmed out, or unsteady. Doctors call this orthostatic hypotension, also known as postural hypotension. [1][2]
That term sounds technical, but the idea is simple: your body had a harder-than-usual time adjusting to standing.
Common reasons this happens
1. Dehydration
This is one of the most common reasons, especially in older adults. If you have not had enough to drink, or if you have been sweating, vomiting, had diarrhea, or a fever, your blood volume can drop. That makes it harder for your body to maintain steady blood pressure when you stand. [1][2]
Many people do not realize how easily mild dehydration can make this symptom worse.
2. Blood pressure medication
If you take medication for high blood pressure, this is an important possibility to consider. Drugs such as ACE inhibitors like lisinopril, water pills such as hydrochlorothiazide, and some calcium channel blockers can lower blood pressure enough to make standing feel harder. [2][4]
That does not mean the medication is wrong for you. It may mean the dose, timing, or combination needs review. Do not stop a prescribed medication on your own. Bring it up with your clinician instead. [4]
3. Other medications
Blood pressure medicines are not the only ones that can do this. Antidepressants, alpha-blockers used for prostate symptoms, nitrates, and some Parkinson's medications can also contribute. [1][3]
A good question to ask yourself is: did this start after a new medication, a dose increase, or a change in when I take it?
4. Being still for too long
You may notice this more after getting out of bed, standing up after a long car ride, or rising too quickly after sitting for a while. It can also happen more often after illness or surgery, when your body is a little deconditioned. [1][3]
5. Low blood sugar, anemia, or recent illness
Sometimes dizziness on standing is a clue that something else is going on. Low blood sugar can make you feel shaky or faint, especially if you have diabetes. Anemia can reduce oxygen delivery and leave you weak or lightheaded. Viral illness, poor appetite, or recovery after being sick can also make these episodes more likely. [2][3]
6. Less common but more serious causes
Sometimes recurring dizziness on standing is linked to a heart rhythm problem, a heart condition, blood loss, or a nervous system disorder that affects blood pressure control. [1][2][3] These are less common, but they are exactly why repeated episodes deserve attention.
What to do right away when it happens
- Sit or lie down right away.
- Hold onto something stable if you need to.
- Take a few slow breaths and give it a moment to pass.
- Drink some water if you may be dehydrated.
- The next time you stand, do it in stages: sit up first, pause, then stand slowly.
- Avoid stairs, driving, or anything that could be dangerous until you feel normal again.
If you actually faint, nearly faint, or hit your head, do not ignore it. Even if you feel better afterward, it should be discussed with a medical professional.
When dizziness is an emergency
Seek emergency help right away if dizziness comes with any of the following: [1][2]
- Chest pain or pressure
- Severe shortness of breath
- Fainting or loss of consciousness
- Trouble speaking
- Sudden confusion
- Weakness or numbness on one side
- A severe new headache
- Blood in your vomit or stool
- Signs of severe dehydration or shock
Those symptoms can point to something more serious than a simple blood pressure dip.
When to make a doctor's appointment
You should make an appointment if:
- This is happening often
- It started after a medication change
- You have fallen or nearly fallen
- You have diabetes, heart disease, or high blood pressure
- The episodes are lasting longer
- It seems to be getting worse over time
- You are avoiding activities because you are afraid it will happen again
Frequent dizziness is not just uncomfortable. It can also increase the risk of falls, especially in older adults. [3]
If you take blood pressure medication
This deserves its own section because it is so common.
If you take lisinopril, amlodipine, a diuretic, or a combination blood pressure pill, dizziness after standing may be related to the medication, especially if:
- You recently started it
- Your dose changed
- You have not been drinking enough
- You have been sick
- You are taking more than one blood pressure-lowering medicine
A helpful way to bring this up is: "I'm getting dizzy when I stand up. Could my medication, dose, or timing be part of the reason?" That gives your clinician something concrete to work with.
What to track before your appointment
Your doctor will want specifics. If this has been happening more than once, write down:
- What time of day it happens
- Whether it happens after meals, after getting out of bed, or after taking medication
- How long the dizziness lasts
- Whether you actually fainted or only felt close to fainting
- Your sitting and standing blood pressure, if you monitor at home
- How much water you've been drinking
- Any new medications or dose changes
- Any other symptoms like nausea, blurry vision, palpitations, weakness, or shortness of breath
That small log can be genuinely useful.
How doctors usually figure out the cause
A clinician may:
- Review your symptoms and medication list
- Check your blood pressure while lying down and then standing [1][3]
- Ask when it happens, how long it lasts, and whether you faint
- Order blood tests if anemia, dehydration, or low blood sugar is a concern [1]
- Do heart testing if your symptoms suggest a rhythm problem or another cardiac issue
That is why details matter. The more specific you are, the easier it is to find the cause.
Frequently asked questions
Is brief dizziness when standing normal?
A short wave of lightheadedness that lasts only a few seconds can happen from time to time and may not mean anything serious. But if it happens often, makes you feel unsafe, or leads to falls, it is worth getting checked. [1][3]
Can lisinopril cause dizziness when standing?
Yes. Lisinopril and other blood pressure medicines can contribute to dizziness or lightheadedness, especially when starting treatment, increasing the dose, or becoming dehydrated. [4]
Is this the same as vertigo?
Not usually. Vertigo tends to feel like spinning or motion, often from an inner-ear problem. Dizziness from standing is more of a faint, washed-out, or unsteady feeling tied to position change and blood pressure. [3]
The bottom line
Feeling dizzy when you stand up is common, and often the cause is something manageable, like dehydration or medication-related blood pressure changes. But common does not always mean harmless.
If it is happening repeatedly, affecting your balance, or coming with warning signs, do not just try to power through it. Talk to your doctor. A careful review of your symptoms, medications, and blood pressure may be enough to find the reason and help you feel steadier again.
Still not sure what might be causing it?
MediCare AI searches trusted medical sources and gives you a personalized answer based on your health profile.
Download MediCare AISources
- Mayo Clinic. "Orthostatic hypotension (postural hypotension) - Diagnosis & treatment." mayoclinic.org
- Cleveland Clinic. "Low Blood Pressure (Orthostatic Hypotension)." clevelandclinic.org
- American Academy of Family Physicians. "Orthostatic Hypotension: A Practical Approach." aafp.org
- MedlinePlus. "Lisinopril." medlineplus.gov
This article is for educational purposes only and does not replace professional medical advice, diagnosis, or treatment. If you are experiencing symptoms, consult a qualified healthcare provider.
